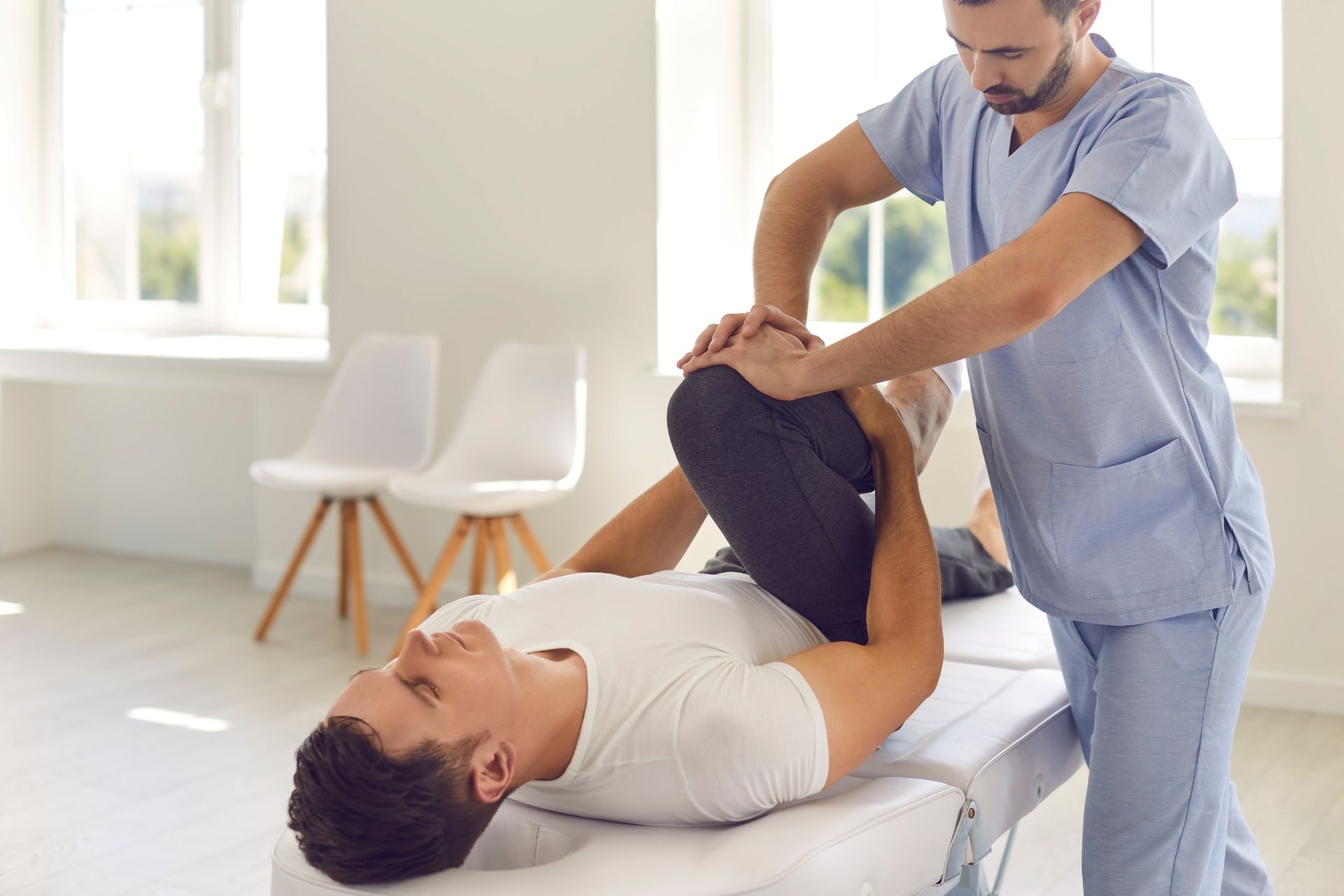
Soft Tissue Manipulation
How does soft tissue manipulation help in reducing muscle tension and improving flexibility?
Soft tissue manipulation, such as massage therapy, can help reduce muscle tension and improve flexibility by targeting specific areas of the body where tension has built up. By applying pressure and manipulating the soft tissues, therapists can release tight muscles and fascia, allowing for increased range of motion and flexibility. This can also help improve blood flow to the muscles, aiding in their recovery and overall health.